Steven Green, a fourth-year medical student at the WSU Elson S. Floyd College of Medicine who hails from the rural Kitsap Peninsula, is putting a national spotlight on how the MD program’s curriculum equips students with hands-on surgical experience in rural Washington communities. The clerkship experiences offer unique training opportunities and may help recruit future physicians to the communities that need them most.
Green was competitively selected to present at the 2026 North American Rural Surgical Society (NARSS) annual meeting held in San Diego, California, last month. He discussed his own clinical experiences and presented the findings of his study on surgical procedures students participate in at urban versus rural sites. Hands-on surgical experiences in rural settings and promising frontiers like robotic surgery may help solve the surgeon shortages facing many rural communities.
Rural Surgery: A Hands-on Environment for Medical Students
WSU’s MD program includes required clinical experiences, or clerkships, in rural and medically underserved areas of Washington. While U.S. medical schools have historically hosted surgical clerkships at large urban medical centers, where resident physicians supervise medical students, the WSU College of Medicine’s community-based model places students at hospitals and clinics across Washington, where they train with experienced physicians.
“I often worked directly with surgeons, rather than with resident trainees, and this gave me hands-on experience,” Green said of his third-year longitudinal integrated clerkship (LIC). Instead of traditional block rotations, the LIC model integrates exposure to multiple disciplines throughout the year to ensure continuity and foster skills development over time. Green was assigned to the Vancouver clinical region and completed three two-week surgical “spotlights” during the year.
Green also presented the results of a study comparing surgical experiences medical students report observing or participating in at urban versus rural sites. He found that students at rural sites logged similar types of general surgical procedures compared to students at urban sites, but with subtle differences in how often they observed versus participated in the procedures.
While observation-only time occurred more often in rural settings, when a student in a rural clerkship was invited to participate, hands-on instrument time was significantly higher in rural compared urban settings. Students in rural settings reported spending 75–100% of the case’s total time holding (and presumably using) surgical instruments, reflecting high engagement and trust from supervising physicians.
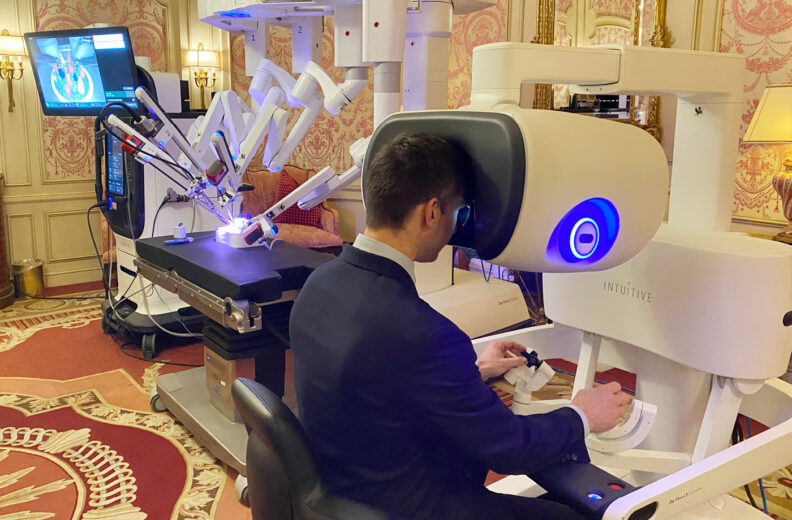
Robotic Surgery: New Frontiers in Care in Rural Settings
Vice Chair of Surgery Anjali Kumar, MD MPH, who is senior author on the study, plans to take Green’s work a step further to study how robotic surgery technology affects medical student engagement. She and her team, which includes third-year WSU medical student Ali Schroeder and College of Medicine data scientist Jessica (Groven) Arends, will use the case log data to look at robotic surgery in educational settings.
Faced with a shrinking surgery workforce, rural and underserved communities stand to gain the most from the implementation of robotic surgery. Robotic arms allow one surgeon to execute procedures that would otherwise require multiple people on hand.
Surgical robots may help attract talented surgeons to rural areas in addition to improving efficiency and patient outcomes, notes South Dakota-based surgeon Gary Timmerman, MD, FACS, who attended the NARSS meeting. He has championed rural surgical issues as a regent of the American College of Surgeons.
Future of the Physician Workforce: Recruiting Rural Surgeons
Green is one of more than a dozen fourth-year medical students at the College of Medicine planning to pursue a career in surgery. Educators and physicians hope exposure to rural settings will encourage newly-minted surgeons to practice in rural communities, which face an acute and worsening shortage of surgeons.
“We need to train from the ground up. We know from research that exposure to rural rotations in medical school and residency really increases the likelihood that someone will return to a rural area,” said Lauren Smithson, MD, a frontier surgeon from Newfoundland, Canada, and chair of the American College of Surgeons’ Advisory Council for Rural Surgery.
Smithson will speak at the MD program’s Transition to Residency surgery course in April.
This article was written by Alex Anderson.
