
Curriculum by Program Year
Clerkship Years: Clinical Immersion and Specialization
In the final two years of medical school, the primary focus of the program shifts from classroom learning to learning in the clinical setting. As a junior member of health care teams in outpatient and inpatient settings, you will put your foundational medical science knowledge and clinical training into practice diagnosing and treating patients, closely supervised by practicing physicians.
You and your fellow students will relocate to your respective regional campuses to gain clinical experiences at community hospitals and clinics, starting with the Year 3 Longitudinal Integrated Clerkship. Year 4 consists of a four-week sub-internship in one of six core disciplines, a four-week Emergency Medicine rotation, a four-week underserved rotation in the rural or urban setting, and 24 weeks of elective rotations.
Work Closely with Top Clinicians in the Community
In our community-based medical education model, you will complete most of your clinical training in community clinics and hospitals throughout Washington and beyond, learning from practicing physicians and other health care professionals.
Students who receive community-based training report numerous benefits, including increased hands-on experience, frequent feedback, and a true sense of companionship with preceptors. Through the community-based model, you will acquire the confidence and expertise of a resident long before beginning your residency.
Year 3
The third year consists of a Longitudinal Integrated Clerkship (LIC) at your regional campus. Clerkships expose students to various aspects of patient care, allowing them to develop their clinical skills through hands-on experiences. You will increase your competency in clinical skills including taking histories, conducting physical examinations, formulating diagnoses, documenting encounters, writing orders, performing procedures, and communicating with patients, families, and colleagues.
Students gain clinical experience in six clinical care domains during the LIC
- Care of the Ambulatory Adult Patient
- Care of the Hospitalized Patient
- Care of the Patient with Obstetric or Gynecologic Needs
- Care of the Patient with Psychiatric Needs
- Care of the Pediatric Patient
- Care of the Surgical Patient
A New and Innovative Approach to Clinical Training
Longitudinal Integrated Clerkships have numerous advantages compared to traditional block clerkships. While a block clerkship focuses on one clinical domain for a set period before rotating to another, the LIC incorporates multiple clinical domains over the course of a year, allowing students to form deeper relationships with patients and preceptors and hone clinical skills over a longer period of time.
Year 4
In the final year of the program, students continue immersive and increasingly personalized clinical experiences through a sub-internship, required rotations, and elective rotations, learning more advanced clinical skills and focusing their attention on a particular primary care domain or specialty of interest.
Students choose a sub-internship and elective rotations to suit their educational and professional goals. For example, if you want to become a pediatrician, you may choose a pediatrics sub-internship and electives in neonatology, adolescent medicine, and pediatric emergency medicine.
Emergency Medicine, Sub-Internship, Underserved Rotations
Students complete 12 weeks of clinical rotations in the following:
- Emergency Medicine rotation for four weeks.
- Sub-internship rotation: This is a clinical experience similar to a traditional block clerkship rotation, but with additional responsibilities for students as they practice under the supervision of a physician. The sub-internship will help prepare you for your internship, which is the first year of residency.
Students choose one of six disciplines for their four-week sub-internship
- Family Medicine
- General Surgery
- Internal Medicine
- Obstetrics and Gynecology
- Pediatrics
- Psychiatry
Students also complete a four-week rotation in the care of underserved populations in either a rural or urban environment, in alignment with the college’s mission to serve Washington’s underserved communities.
Elective Rotations in Patient Care, Research, or other Learning Experiences
Students can choose from over 100 options to complete a total of 24 weeks of electives in Year 4. These include rotations in most medical specialties and varied health care settings, domestic and international away rotations, research activities, and virtual courses. Students may also design their own rotation to take with administrative approval.
Applying to Residency Programs
During the first part of the fourth year, students submit residency program applications through the National Residency Matching Program to continue training in their clinical domain of interest after earning their medical degree. You are allocated time during Year 4 to travel for residency interviews.
Licensing Exam, Part 2 of 3
During the fourth year, students also take the second part of the USMLE. This part of the exam tests your understanding of clinical knowledge. The third part of the exam, which tests your ability to practice unsupervised, is typically taken during the first year of residency.
MD Program Curriculum Schematic 2025–2026
Pre-Clerkship Phase
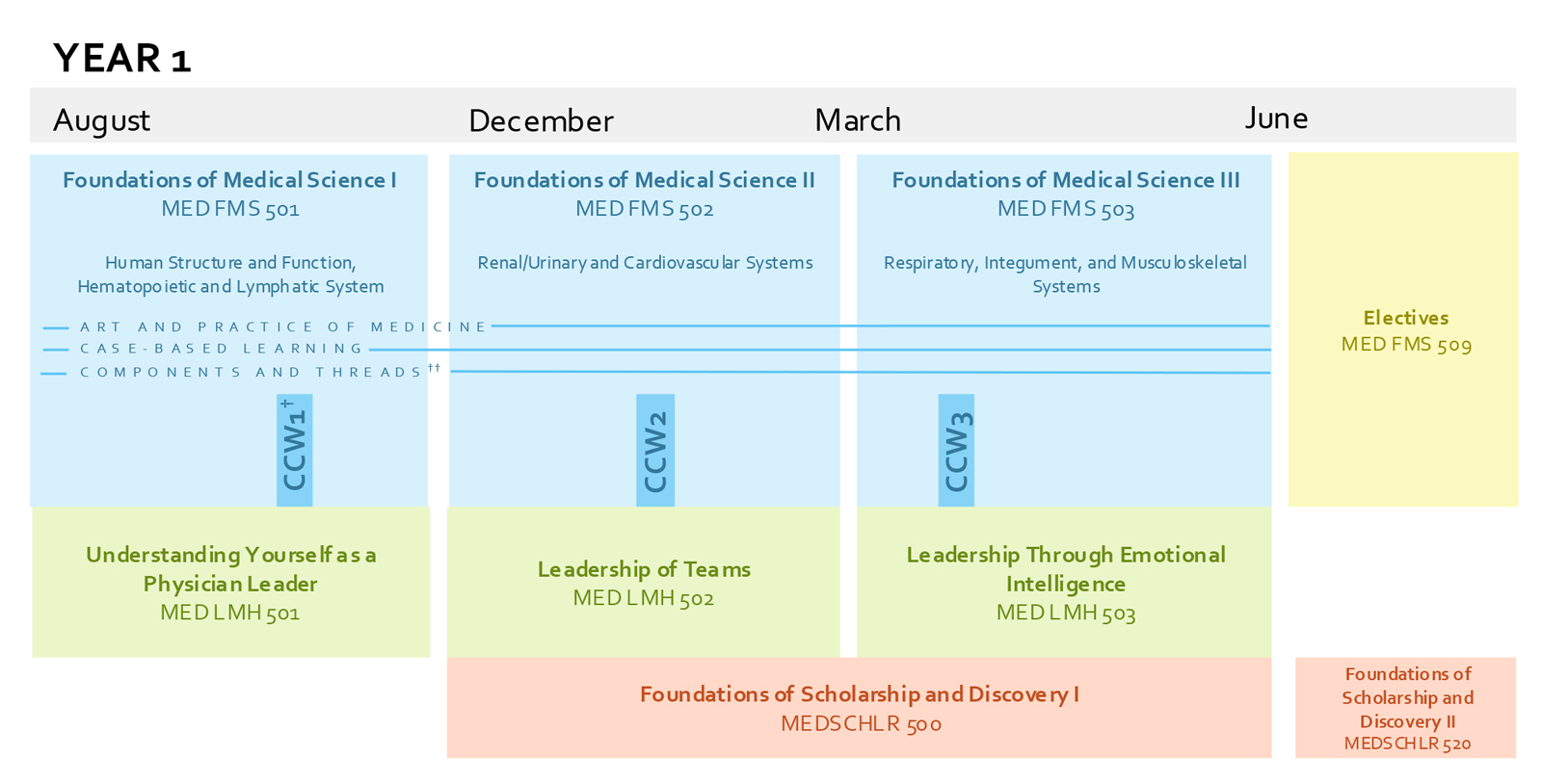
†CCW: Clinical Campus Week.
††Threads: Anatomy, Mind and Behavior, Cardiovascular, Cellular/Molecular Science, Community Engagement, Digestive/Gastroenterology, Endocrine, Ethics, Health Equity, Hematopoietic, Histology, Immunology, Integumentary, Interprofessional Education, Microbiology and Infectious Disease, Musculoskeletal, Neuroanatomy, Neurology, Nutrition, Pathology, Pharmacology, Physiology, Population and Community Health, Radiology, Renal/Urinary, Reproductive, Respiratory, Rheumatology, Service Learning
Year 1 runs from August to July. The first term runs from August through mid-November and contains two courses: Foundations of Medical Science I (MED FMS 501) and Understanding Yourself as a Physician Leader (MED LMH 501). MED FMS 501 focuses on Human Structure and Function and the Hematopoietic and Lymphatic systems. Clinical Campus Week 1 occurs about halfway through the course.
The second term begins in mid-November and ends in mid-March. Foundations of Medical Science II (MED FMS 502) focuses on the Renal/Urinary and Cardiovascular systems, as well as the first portion of the Respiratory system. Clinical Campus Week 2 occurs roughly halfway through the term. The leadership course is called Leadership of Teams (MED LMH 502). A new course is added, called Foundations of Scholarship and Discovery I (MEDSCHLR 500); this course runs from November until Mid-June.
The third term begins in March and ends in June. Foundations of Medical Science III (MED FMS 503) completes the Respiratory system before moving to the Integument and Musculoskeletal systems. Clinical Campus Week 3 occurs towards the beginning of the term. The leadership course is called Leadership Through Emotional Intelligence (MED LMH 503). As mentioned above, MEDSCHLR 500 continues in this term.
The fourth term begins in June and ends in August. Students may optionally enroll in electives (MED FMS 509) or Foundations of Scholarship and Discovery II (MEDSCHLR 520) during this term.
Pre-Clerkship Phase
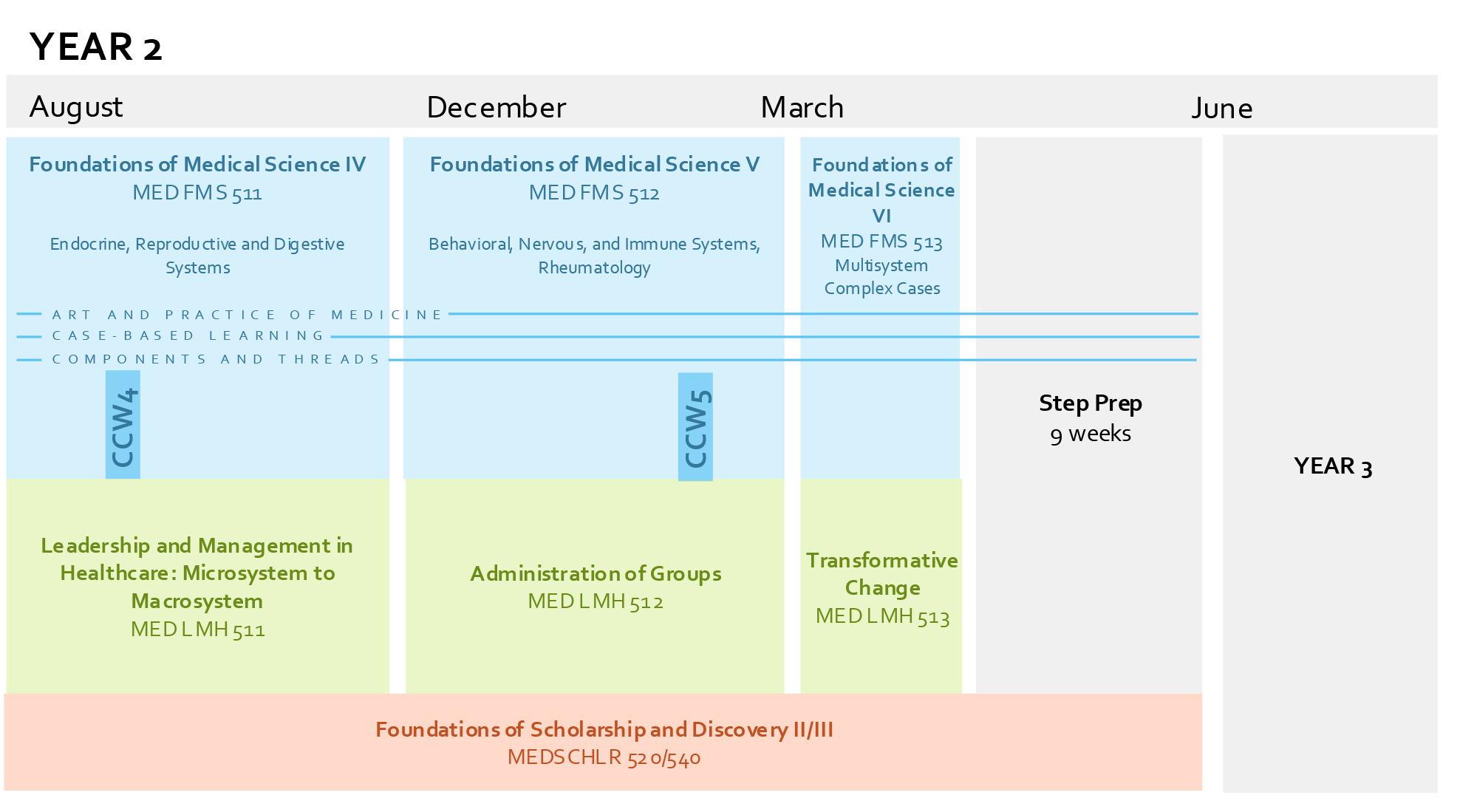
†CCW: Clinical Campus Week.
††Threads: Anatomy, Mind and Behavior, Cardiovascular, Cellular/Molecular Science, Community Engagement, Digestive/Gastroenterology, Endocrine, Ethics, Health Equity, Hematopoietic, Histology, Immunology, Integumentary, Interprofessional Education, Microbiology and Infectious Disease, Musculoskeletal, Neuroanatomy, Neurology, Nutrition, Pathology, Pharmacology, Physiology, Population and Community Health, Radiology, Renal/Urinary, Reproductive, Respiratory, Rheumatology, Service Learning
Year 2 runs from August to June. The first term runs from August through mid-November. Foundations of Medical Science IV (MED FMS 511) contains the Endocrine, Reproductive, and Digestive Systems. Clinical Campus Week 4 occurs towards the beginning of the term. The leadership course is called Leadership and Management in Healthcare: Microsystem to Macrosystem (MED LMH 511). Students may optionally enroll in Foundations of Scholarship and Discovery II (MEDSCHLR 520) or Foundations of Scholarship and Discovery III (MEDSCHLR 540). Both courses run from August through June.
The second term begins in mid-November and ends in mid-March. Foundations of Medical Science V (MED FMS 512) focuses on the Behavioral, Nervous, and Immune Systems, as well as Rheumatology. Clinical Campus Week 5 occurs towards the end of the term. The leadership course is called Administration of Groups (MED LMH 512). As mentioned above, MEDSCHLR 520 and 540 continue in this term.
The third term begins in Mid-March and ends in June. Foundations of Medical Science VI (MED FMS 513) provides a 4-week focus on multisystem complex cases before breaking for 8 weeks of dedicated time for USMLE Step 1 and relocating to the student’s assigned regional campus. There is no clinical campus week in this term. The leadership course is Transformative Change (MED LMH 513). As mentioned above, MEDSCHLR 520 and 540 continue in this term.
Years 1 and 2 also contain longitudinal elements that are delivered throughout the MED FMS courses called Art and Practice of Medicine and Case-Based Learning. Similarly delivered elements throughout these courses are called Components and Threads and include: Anatomy, Mind and Behavior, Cardiovascular, Cellular/Molecular Science, Community Engagement, Digestive/Gastroenterology, Endocrine, Ethics, Health Equity, Hematopoietic, Histology, Immunology, Integumentary, Interprofessional Education, Microbiology and Infectious Disease, Musculoskeletal, Neuroanatomy, Neurology, Nutrition, Pathology, Pharmacology, Physiology, Population and Community Health, Radiology, Renal/Urinary, Reproductive, Respiratory, Rheumatology, Service Learning.
Clerkship Phase
†Required Selective
- Rural Underserved Medicine – MED CLIN 538
- Urban Underserved Medicine – MED CLIN 539
(may be completed any time in year 4)
††Required Selective – Sub-Internship
- Family Medicine – MED CLIN 531
- Internal Medicine – MED CLIN 532
- Surgery – MED CLIN 533
- Pediatrics – MED CLIN 534
- Psychiatry – MED CLIN 535
- Obstetrics and Gynecology – MED CLIN 536
(may be completed any time in year 4)
*Required Clerkships
- Longitudinal Integrated Clerkship – MED CLIN 521-524
- Emergency Medicine – MED CLIN 537
**Electives
MED CLIN 530-638, 2-4 week rotations
24 credit hours required for graduation
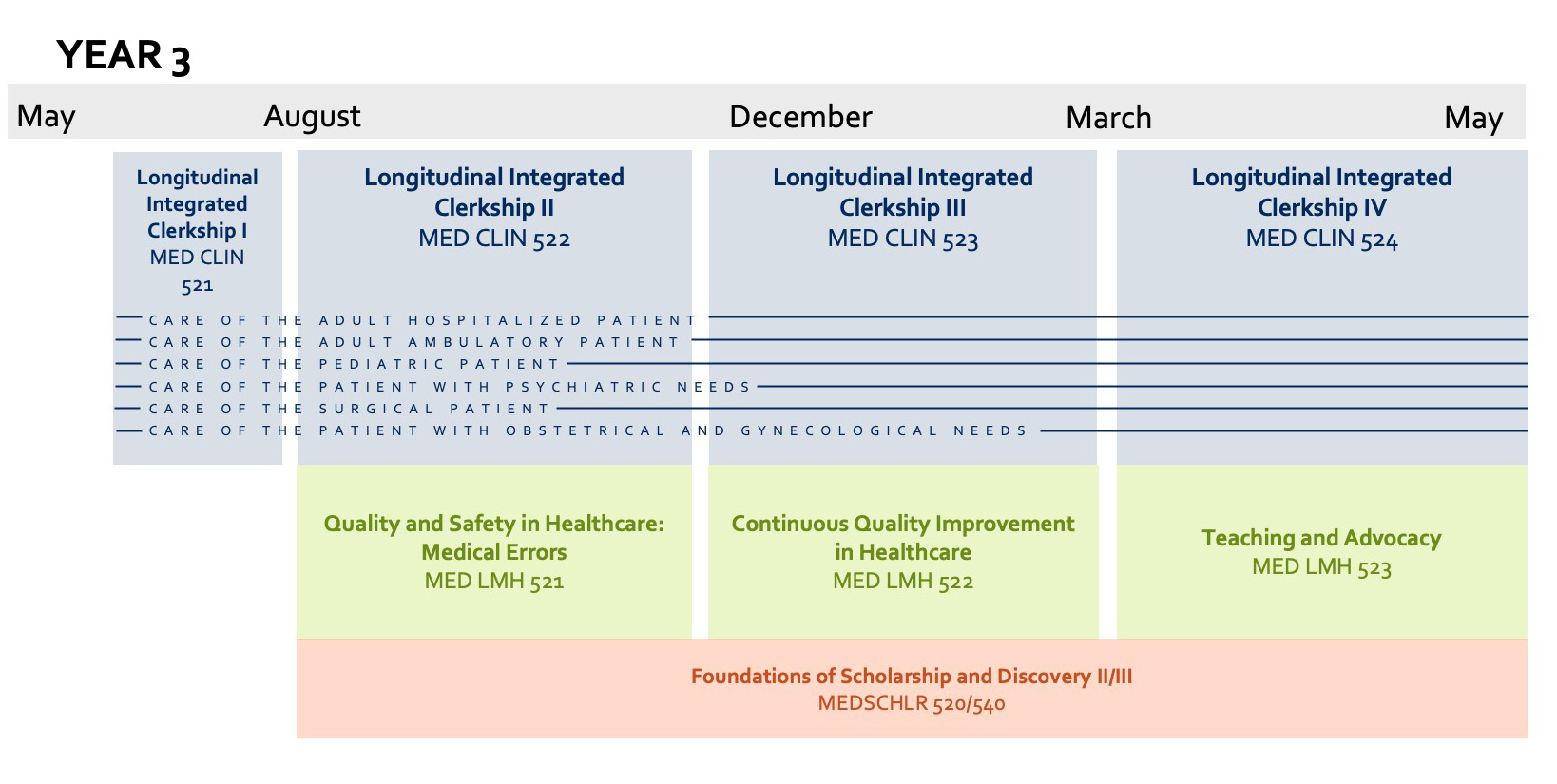
Year 3 begins in mid-June and runs through May. The first term is June through mid-August and only contains the Longitudinal Integrated Clerkship I course (MED CLIN 521). Similar to the longitudinal elements that run throughout the MED FMS courses are six care domains that are embedded in these Year 3 MED CLIN courses:
- Care of the Adult Hospitalized Patient
- Care of the Adult Ambulatory Patient
- Care of the Pediatric Patient
- Care of the Patient with Psychiatric Needs
- Care of the Surgical Patient
- Care of the Patient with Obstetrical and Gynecological Needs
The second term is mid-August through mid-November. Longitudinal Integrated Clerkship II (MED CLIN 522) occurs with the continuation of the care domains. The leadership course is called Quality Safety in Healthcare: Medical Errors (MED LMH 521). Like in Year 2, students may optionally enroll in Foundations of Scholarship and Discovery II (MEDSCHLR 520) or Foundations of Scholarship and Discovery III (MEDSCHLR 540). Both courses run from August through May.
The third term is mid-November through mid-March. Longitudinal Integrated Clerkship III (MED CLIN 523) occurs with the continuation of the care domains. The leadership course is called Continuous Quality Improvement in Healthcare (MED LMH 522). MEDSCHLR 520 and 540 continue as mentioned above.
The fourth term is mid-March through May. Longitudinal Integrated Clerkship IV (MED CLIN 524) occurs with the continuation of the care domains. The leadership course is called Teaching and Advocacy (MED LMH 523). MEDSCHLR 520 and 540 end at the conclusion of this term. Students must completed MEDSCHLR 520 by the end of their third year.
Clerkship Phase
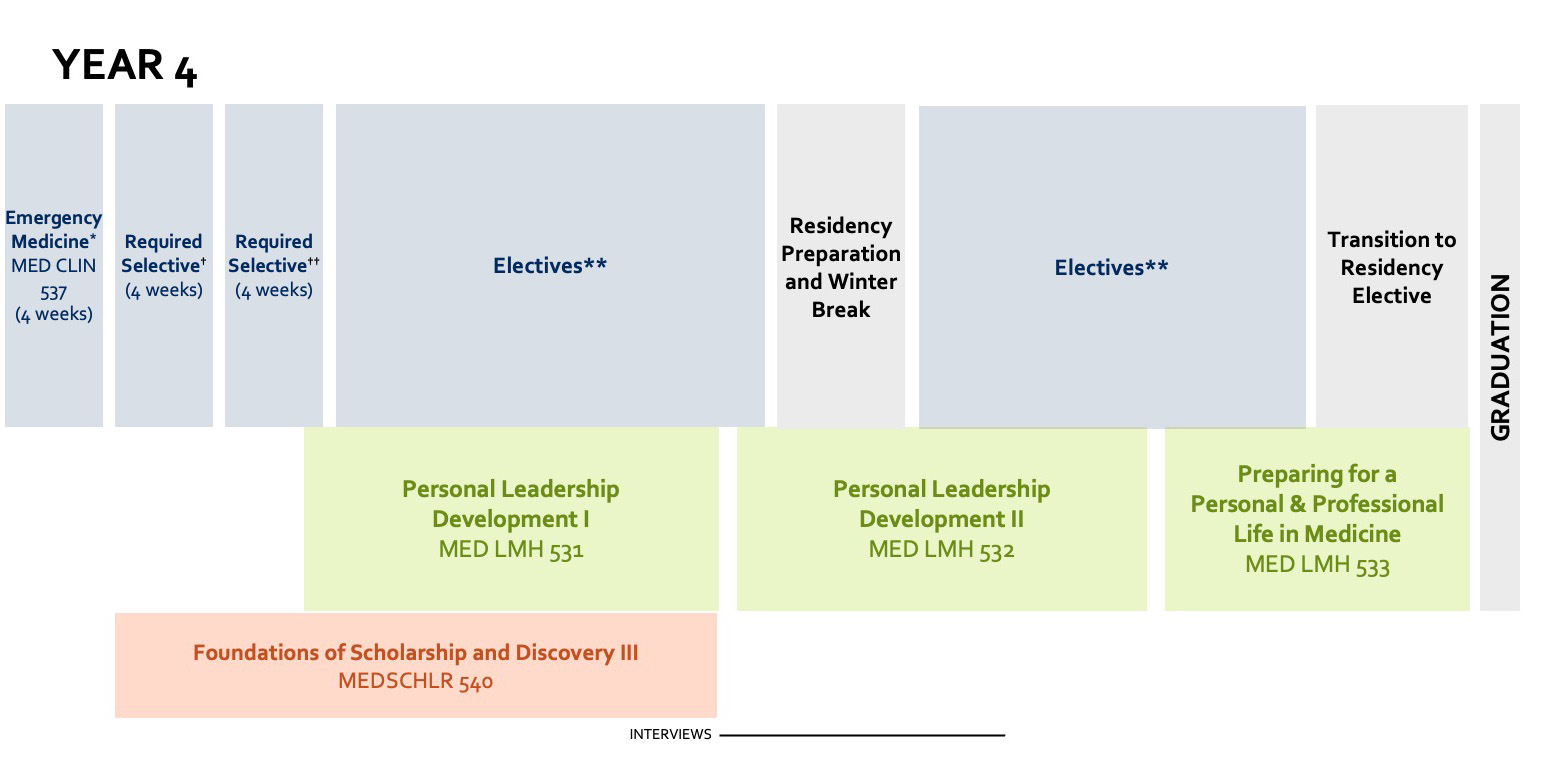
†Required Selective
- Rural Underserved Medicine – MED CLIN 538
- Urban Underserved Medicine – MED CLIN 539
(may be completed any time in year 4)
††Required Selective – Sub-Internship
- Family Medicine – MED CLIN 531
- Internal Medicine – MED CLIN 532
- Surgery – MED CLIN 533
- Pediatrics – MED CLIN 534
- Psychiatry – MED CLIN 535
- Obstetrics and Gynecology – MED CLIN 536
(may be completed any time in year 4)
*Required Clerkships
- Longitudinal Integrated Clerkship – MED CLIN 521-524
- Emergency Medicine – MED CLIN 537
**Electives
MED CLIN 530-638, 2-4 week rotations
24 credit hours required for graduation
Year 4 begins at the end of May and runs through early May the next year. During Year 4, students transition to an individualized rotation-based schedule and are required to complete a required four-week clinical rotation in Emergency Medicine (MED CLIN 537) and a four-week selective clinical rotation in either Rural Underserved Medicine (MED CLIN 538) or Urban Underserved Medicine (MED CLIN 539). Students are also required to complete a four-week selective in one of the following clinical disciplines:
- Family Medicine (MED CLIN 531)
- Internal Medicine (MED CLIN 532)
- Surgery (MED CLIN 533)
- Pediatrics (MED CLIN 534)
- Psychiatry (MED CLIN 535)
- Obstetrics and Gynecology (MED CLIN 536)
In addition to these required rotations that must be completed during Year 4, students must complete electives from the MED CLIN 530-638 course series. These electives may be 2-4 week rotations, and students are required to complete 24 credit hours to graduate. Time is blocked in December to represent residency preparation and winter break, with residency interviews occurring from mid-November through early February.
The leadership courses are offered on the term schedule, with Personal Leadership Development I (MED LMH 531) offered in the second term from August through mid-November. Personal Leadership Development II (MED LMH 532) is offered in the third term from mid-November through mid-March. The final leadership course, Preparing for a Personal & Professional Life in Medicine (MED LMH 533) is offered in the last term from mid-March through the beginning of May.
Foundations of Scholarship and Discovery III (MEDSCHLR 540) is offered through the first and second term of year 4, from mid-June through mid-November. Students are required to complete MEDSCHLR 540 by the end of their fourth year.
A two-week Transition to Residency elective is offered in April. The end of Year 4 is marked by graduation, which occurs in early May.